 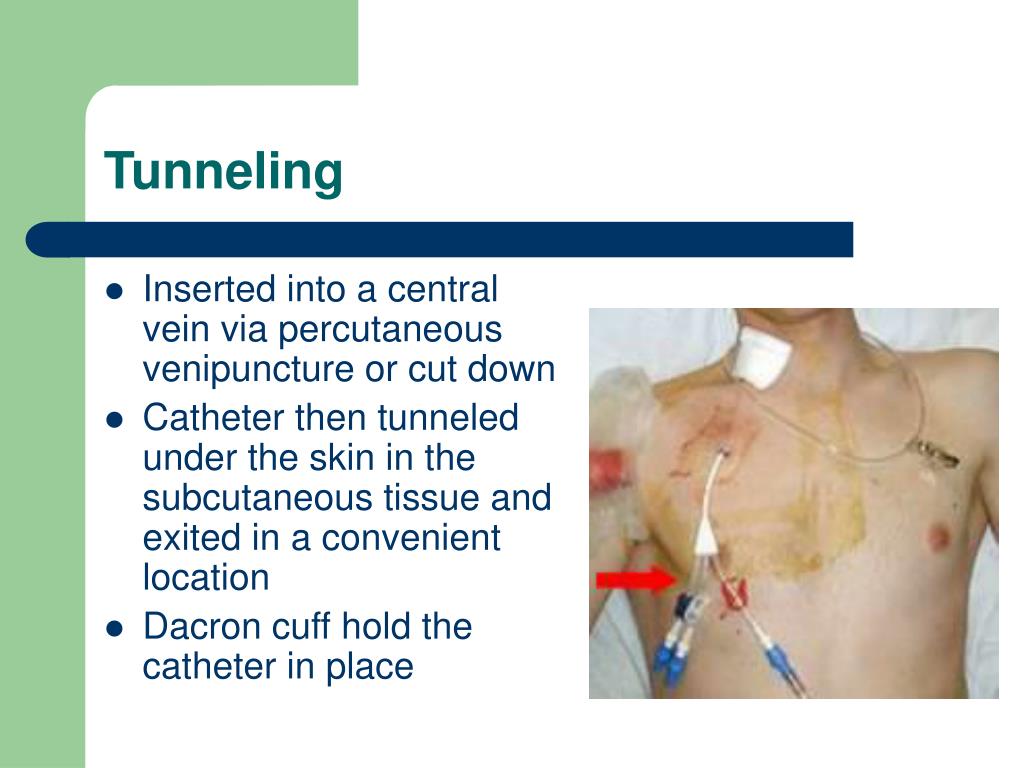
14, 17-19, 22-25 Features of the CVC associated with increased rates of CRT include: PICC > centrally inserted catheter > implanted port, 14, 17-19 jugular > subclavian, 24 size of the catheter relative to the size of the vein, 3, 14, 20 and position of the catheter tip. Risk factors for CRT can be divided into those related to the catheter or its insertion and factors related to the patient ( Table 2). 20 In another study of 2056 PICCs placed over 1 year, symptomatic UEDVT and SVT were detected in only 2.6% and 2.0%, respectively. Among 332 patients randomized to 1 of 2 PICCs who underwent DUS at catheter removal or at 28 days, thrombosis was detected in 72%, whereas symptomatic DVT occurred in only 4%. 
3 In patients with a PICC (as with other CVCs), there is a major disconnect between asymptomatic DVT detected by screening and symptomatic DVT. 19 This may be related to their longer length, greater catheter-to-arm vein diameter, and increased mobility of the catheter with subsequent endothelial injury. 14, 17-21 A review of 11 studies in almost 4000 patients found that PICCs were associated with a 2.6-fold greater risk of thrombosis than other types of CVC ( P <. 16 However, PICCs are associated with an even greater DVT risk than centrally placed catheters. The use of PICCs has increased substantially in recent years because they are easy to insert and remove at the bedside by nurse CVC teams, the risk of early complications is very low, and they can be readily used outside of the hospital. Occasionally, a catheter-tip thrombus will create a ball valve phenomenon that impedes withdrawal of blood from the catheter while instillation of fluids remains possible. 3 Ongoing movement of the catheter within the vein produces endothelial erosions and triggers the development of mural thrombi, which encroach on the lumen until there is occlusion of the vein. Blood flow is reduced up to 60% around the CVC, which leads to further cellular adhesion to the catheter and vein walls. 2 This pericatheter sheath grows along the catheter from the venotomy site. Deposition of fibrin on the thrombogenic catheter surface and the subsequent in-growth of smooth muscle and endothelial cells are universal and begin within hours of insertion. Insertion of a CVC produces local venous injury at the access site. Thrombosis associated with a CVC can be classified into 3 types: pericatheter sheath (“fibrin sleeve”), thrombotic occlusion of the catheter lumen, and mural thrombosis, either superficial (SVT) or deep vein thrombosis (DVT). 1 Thrombosis associated with hemodialysis lines, noncatheter venous devices, and in pediatric patients are not discussed. This chapter focuses on the association between CVC and thrombosis, especially on knowledge acquired since the 2012 ASH Education Book. Furthermore, approaches to the prevention CRT have been disappointing. However, there is considerable uncertainty about the risks, treatment, and prevention of catheter-related thrombosis (CRT) because of substantial study heterogeneity and a paucity of rigorous clinical trials on its management. They are used in most critical care patients, in more than 25% of hospitalized non-intensive care unit patients, and in many outpatients for the infusion of IV fluids, blood products, antibiotics, and chemotherapy agents, as well as for blood sampling. Central venous catheters (CVCs) are indispensable components of therapy in many cancer patients and in those undergoing hemodialysis, parenteral feeding, plasmapheresis, or administration of certain drugs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
